Research
Shared decision making around breast cancer screening
As a medical resident, I realized that many older women have screening mammograms despite few data on the benefits for this population. Therefore, as a research fellow, I used data from the National Health Interview Survey to examine rates of mammography screening among older women. I found that 39% of US women >80 years with short life expectancies and therefore little chance to benefit were screened with mammography, while 38% of women >80 years with greater than 10-year life expectancy were not screened. These findings highlighted the need to improve targeting of mammography screening to older women by life expectancy, and most guidelines now encourage clinicians to consider patient life expectancy when deciding on screening. Curious as to why so many older women with little chance to benefit were screened, I used qualitative methods to study older women’s decision making around mammography screening. I found that while some of the oldest women have strong opinions about whether or not to get screened, most women are influenced by their physicians’ recommendations. Physicians, however, report feeling ill prepared to discuss the benefits and risks of mammography or long-term prognosis with older women.
To improve the quality of older women’s decision making around mammography screening, I developed and evaluated a comprehensive pamphlet decision aid on mammography screening for women >75 years. The decision aid is available on ePrognosis, and was deemed high quality in two independent reviews. In addition, the National Cancer Institute (NCI) designated the decision aid an evidence-based cancer control program. In a large multi-site cluster randomized clinical trial, we found that the decision aid increased older women’s knowledge of mammography’s pros and cons and led to 9% fewer women at low or average risk being screened (51% vs. 60%, p=0.006 [Schonberg et al., JAMA Intern Med., 2020]). However, the decision aid did not support clinician communication around screening, nor did it individualize outcomes of screening based on older women’s health and breast cancer risk. Therefore, we recently developed a web-based conversation aid (called decidetogether.info) to support shared decision-making between women aged 75 and older and their primary care clinicians during an encounter (Schonberg et al., J Am Geriatr Soc., 2025).
In developing my mammography screening decision aid, I learned that older women wanted more information about their breast cancer risk to make informed decisions about mammography screening. Since the Breast Cancer Risk Assessment Tool (BCRAT, a.k.a. “Gail model”) is the most widely available and commonly used breast cancer prediction model, I examined its performance in older women and found that BCRAT overpredicted breast cancer in women >75, especially those with multiple comorbidities. Therefore, we developed a novel model to predict 10-year risk of breast cancer, breast cancer death, and non-breast cancer death among postmenopausal women aged 55 and older using data from the Nurses' Health Study, the Black Women's Health Study, the Women's Health Initiative, and the Multiethnic Cohort. Using this model, we created a risk-based decision tool to help older women with decision making around how often to be screened, when to stop screening, and for those at higher breast cancer risk whether to consider breast cancer prevention medications. I made the risk model and the risk-based decision tool available for use
on the ePrognosis website.
Estimating overall prognosis for older adults
To help clinicians and older adults consider life expectancy in care decisions, I developed and validated an index to predict mortality up to 14 years among U.S. adults aged 65 and older. I helped make my prognostic index publicly available in multiple languages at ePrognosis.org, a website I co-developed and that receives >15K hits per month. My index has also been used in many papers to estimate receipt of screening and other preventive services among older adults by their life expectancy. Most recently, using data from the 2019 National Health Interview Survey, we found that many U.S. adults aged 65 and older with <10-year life expectancy underwent cancer screening with little chance of benefit while many did not receive immunizations with a much shorter time-to-benefit. To help improve individualization of preventive care based on older adults' life expectancy, my mentee, we developed strategies for discussing long-term prognosis with older adults. In addition, I served on the American Society of Clinical Oncology’s (ASCO) guideline panel on geriatric oncology that recommended that oncologists use ePrognosis when deciding on chemotherapy for older adults. Breast oncology practices use my mortality index to personalize cancer treatment recommendations for older adults and in 2026 the National Comprehensive Cancer Network began recommending use of my index to estimate life expectancy when deciding on prostate cancer screening and treatment with older adults.
Shared decision making around breast cancer treatment
To better understand breast cancer outcomes among older women, I examined breast cancer characteristics, treatment and survival among older women using data from the NCI’s linked SEER-Medicare database. I found that women >80 years with Stage I/II breast cancer have tumor characteristics similar to those of women 67-79 years yet receive less aggressive treatment and experience higher breast cancer mortality. In addition, I used SEER-Medicare data to examine the relative survival of women >67 years diagnosed with breast cancer and found that compared to women the same age not diagnosed with breast cancer, a diagnosis of ductal carcinoma in situ (DCIS) or Stage I breast cancer is associated with better survival while a diagnosis of Stage II or higher breast cancer is associated with worse survival. Using these data we also found that 40% of women aged 80 and older with short life expectancy received
radiotherapy after breast conserving surgery for early-stage disease despite little chance of benefit. To better understand older
women’s decision making around breast cancer treatment, I conducted a longitudinal study to examine older women’s
experience and decision-making beginning at the time of a breast biopsy. I followed 164 women >65 years for six months.
Among the 70 women ultimately diagnosed with breast cancer, I found that as women age, they are less likely to engage in
breast cancer treatment decisions despite facing multiple preference-sensitive treatment decisions. Therefore, we developed a workbook decision aid on breast cancer treatment for women aged 70 and older with Stage I, estrogen receptor positive, HER2 negative, breast cancer. We have a NIA R01 to test the effects of this decision aid combined with training breast surgeons in shared decision making in a type 1 hybrid effectiveness implementation trial.
Current Investigations
Below you will find our active research projects; click on any title to view the full study details on ClinicalTrials.gov.
Websites
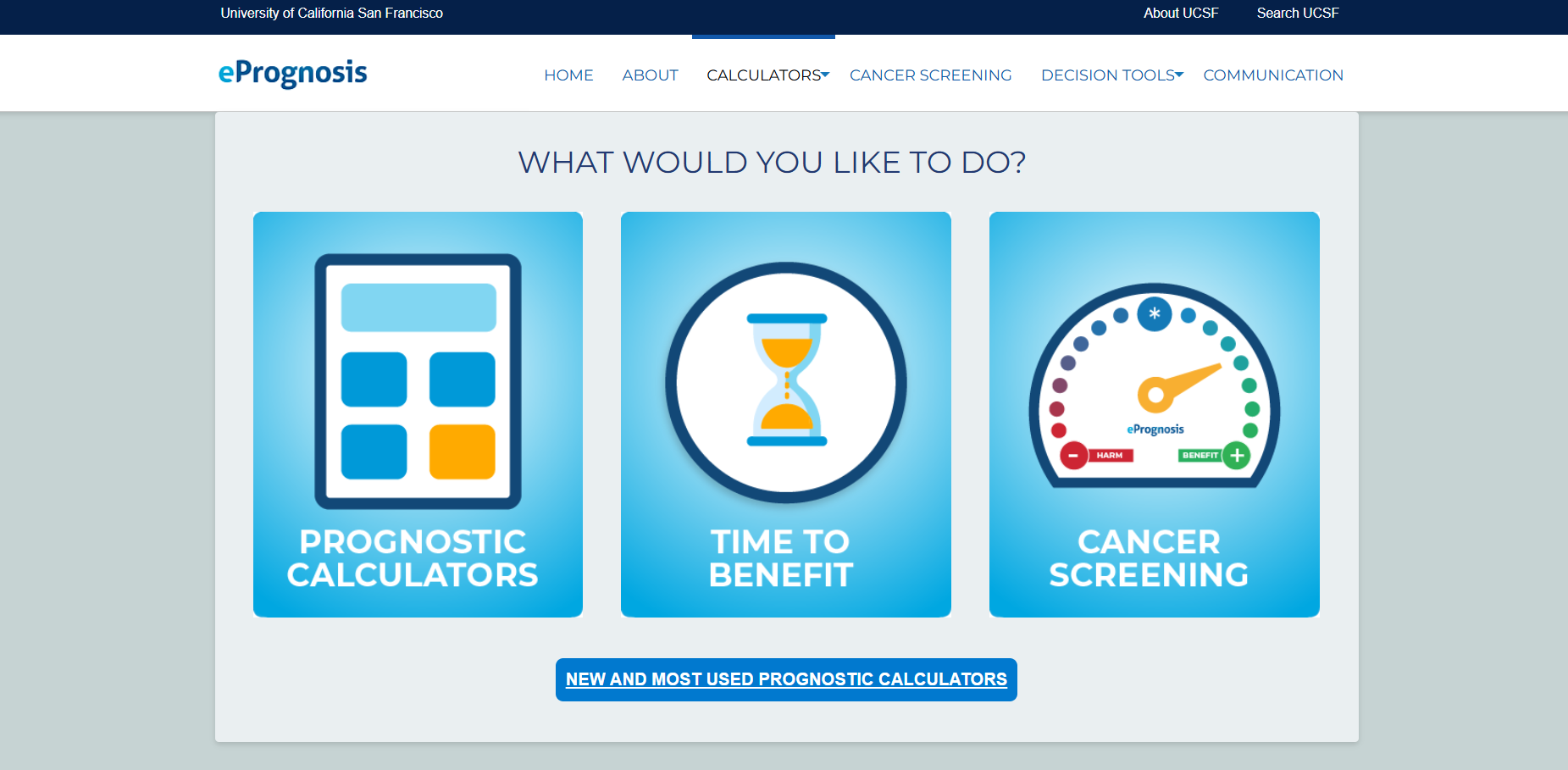
ePrognosis
is an online clinical decision support tool designed to help healthcare professionals navigate the complex process of estimating life expectancy for older adults.
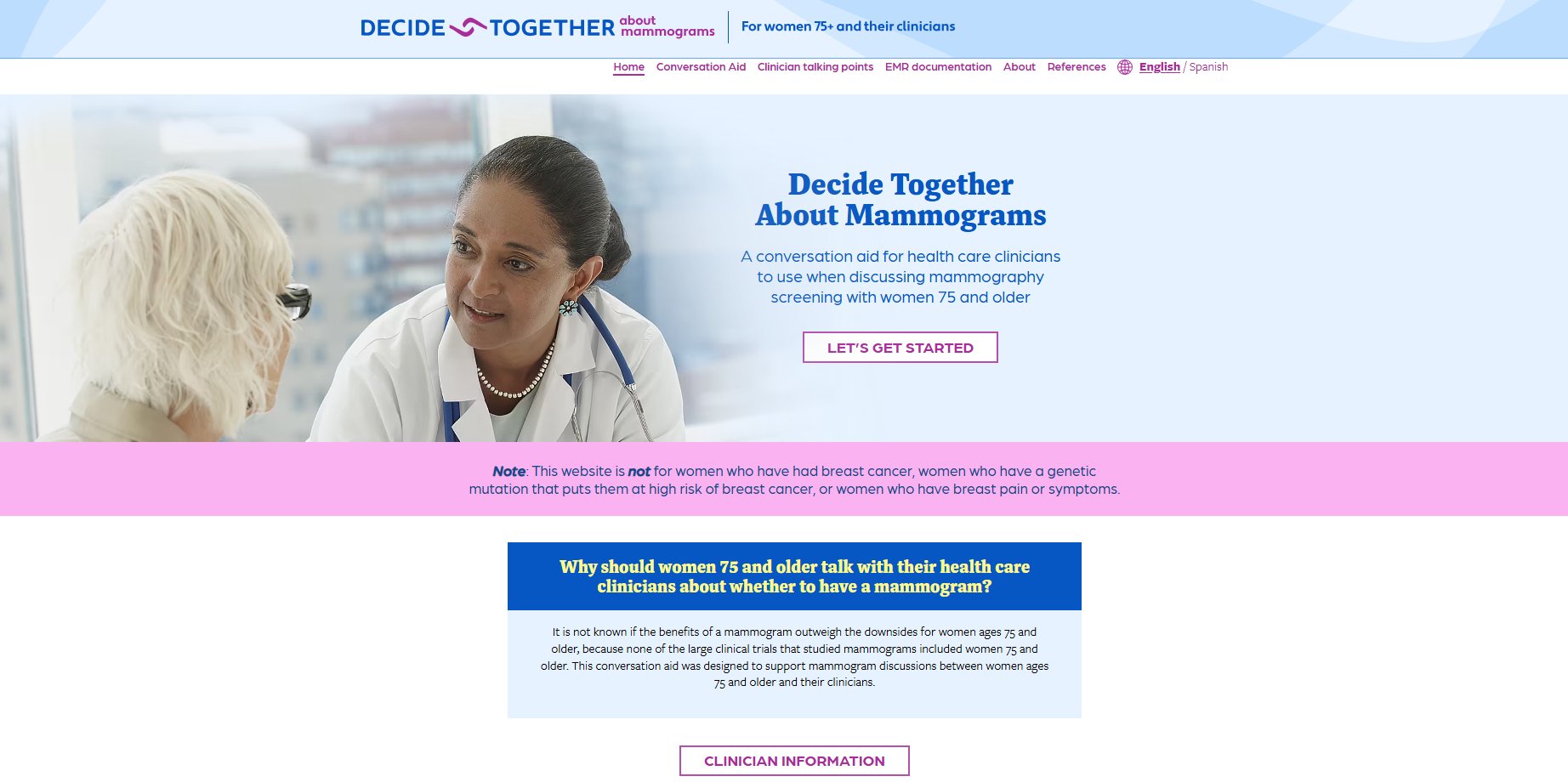
Decide Together
is a clinical conversation aid. It is designed to facilitate shared decision-making between healthcare providers and women aged 75 and older regarding whether to continue routine mammography.
A decision aid for women age 55 and older on breast cancer screening and prevention
This decision aid includes a model that estimates 5 and 10 year breast cancer risk for women ages 55 and older and estimates their 10-year risk of death from causes other than breast cancer. It then provides information on the benefits and risks of mammography screening and breast cancer prevention medications to help women with these decisions.