BACKGROUND: Lymphedema is a prevalent and underserved condition. Expanding diagnostic and therapeutic options have increased interest in multidisciplinary care. This study examines clinical characteristics and geographic patterns of lymphedema care within a multidisciplinary lymphatic center.
METHODS: A retrospective review included all patients evaluated for edema at the BIDMC Lymphatic Center from January 2018 through December 2023. The multidisciplinary team comprised cardiovascular medicine, radiology, plastic surgery, and physical therapy. A RedCap registry captured demographics, clinical characteristics, imaging and surgeries. Patients were stratified by etiology as primary, secondary, or non-lymphatic edema. Bivariate and geospatial analyses assessed differences across groups and geographic access to care.
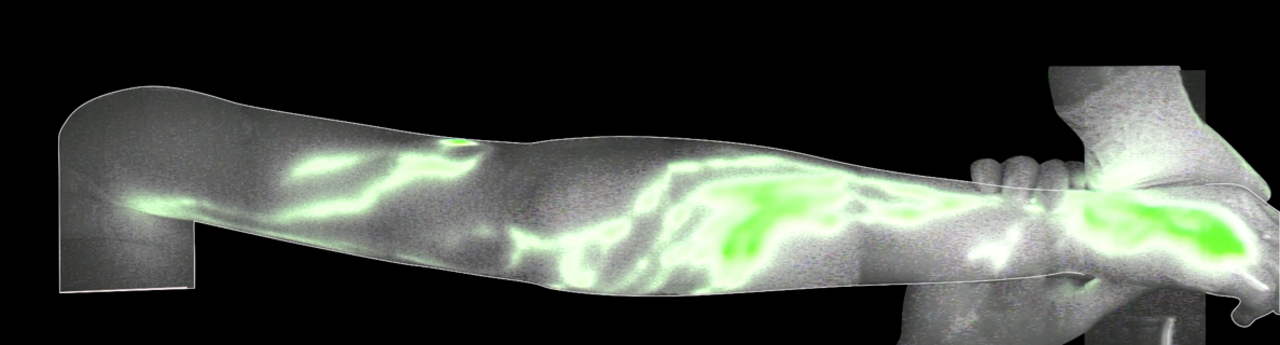
RESULTS: Of the total 2,031 participants, 76% were female, with a mean age of 60 years (±15.2) and BMI of 33.6 kg/m2 (±10.7). The average duration of edema symptoms at evaluation was 9.47 years (±11.8). Secondary lymphedema was most common (n=1,104, 54%), often due to cancer (54%) or chronic venous disease (23%). Lymphatic imaging was performed in 549 patients (27%). Of those 549, lymphoscintigraphy (83%) and MRI (69%) were most common. Only 149 patients (11%) underwent surgery. Patients residing outside the state had longer symptom duration (12.3 vs 9.1 years, p<0.0001) and higher surgical rates (16.6% vs 6%, p<0.001) than those residing in-state.
CONCLUSIONS: In this large, single-center description, over one-third of patients did not have lymphedema. Lymphatic imaging was frequently performed, though few underwent surgery. Geographic barriers delayed evaluation and increased surgical intervention, emphasizing the need for broader access to multidisciplinary lymphatic care.